Emergency physicians spend 44% of every shift on documentation — not patient care. That means nearly half of a 10- or 12-hour ED shift is consumed by clicking, typing, and charting instead of treating the next patient in the queue. In a specialty defined by speed, throughput, and high-stakes decision-making, documentation is the bottleneck that drives burnout, lengthens door-to-disposition times, and increases medicolegal risk.
We ranked 6 AI scribes on the criteria that matter most for emergency medicine documentation:
- Clinical decision support (CDS) — does the AI generate differential diagnoses as a safety net for missed diagnoses?
- MDM documentation for E&M coding — does it structure medical decision making to support 99281-99285 billing?
- Procedure note generation — can it document intubation, central lines, chest tubes, laceration repair, and procedural sedation?
- EHR integration speed — bidirectional write-back to Epic, Cerner, athenahealth before shift change?
All products were evaluated in February-March 2026. Pricing reflects publicly available rates. Enterprise-priced products were assessed based on disclosed ranges and verified customer reports.
Why Emergency Physicians Need an AI Scribe
The Documentation Crisis in Emergency Medicine
Emergency medicine has a documentation problem that is worse than almost any other specialty. Studies from ACEP and the AMA consistently show that emergency physicians spend approximately 44% of their shift time on documentation — charting, ordering, reviewing results, and writing notes — rather than direct patient care. With throughput pressure of 2-4 patients per hour and an average ED visit length of 15-45 minutes, there is almost no margin for documentation inefficiency.
The result is "pajama time" — hours of after-shift charting that extends the workday well beyond the scheduled shift. Emergency physicians routinely spend 1-3 hours completing charts after leaving the department, compounding the physical and cognitive fatigue of high-acuity clinical work. This documentation burden is a primary driver of EM having among the highest burnout rates of any medical specialty, with over 65% of emergency physicians reporting burnout symptoms according to the Medscape Physician Burnout Report.
What General-Purpose AI Scribes Miss in the ED
Most AI medical scribes are built for primary care — 15-minute office visits with a single chief complaint, a focused exam, and a straightforward assessment and plan. Emergency medicine encounters are fundamentally different:
- MDM complexity — Medical decision making for E&M levels 99281-99285 requires documented data reviewed, number and complexity of diagnoses considered, and management complexity including risk of morbidity and mortality. A general-purpose scribe that generates a simple SOAP note does not structure MDM to support the E&M level billed.
- Multi-system undifferentiated complaints — Chest pain in the ED could be cardiac (ACS, aortic dissection), pulmonary (PE, pneumothorax), gastrointestinal (esophageal rupture, pancreatitis), musculoskeletal, or psychiatric (panic attack). The AI must document the full differential workup across organ systems without losing clinical coherence.
- Procedure note requirements — Intubation, central line placement, chest tube insertion, laceration repair, procedural sedation, and lumbar puncture each have required documentation elements: informed consent, timeout, technique and approach, complications, and post-procedure assessment. Most AI scribes have no procedure note capability.
- Disposition and handoff documentation — Structured discharge instructions, admission handoffs using I-PASS or SBAR frameworks, transfer documentation, and inter-facility communication require specific formatting that general-purpose scribes do not support.
- Boarding patient reassessments — When admitted patients board in the ED for hours or days, interval documentation of repeated exams, clinical status changes, and ongoing management decisions is required. The AI must maintain context across reassessment intervals.
Medicolegal Risk — Documentation as Defense
Emergency medicine carries among the highest malpractice rates of any specialty. According to CRICO/Harvard's Comparative Benchmarking System, missed diagnosis is the number one cause of EM malpractice claims — accounting for nearly 40% of all emergency medicine malpractice cases. The most commonly missed diagnoses include myocardial infarction, pulmonary embolism, appendicitis, fractures, and subarachnoid hemorrhage.
In malpractice litigation, the medical record is the primary defense. The legal standard is straightforward: what is not documented did not happen. An AI scribe that generates differential diagnoses alongside the clinical note creates a built-in safety net — documenting that the physician considered and evaluated critical "can't miss" diagnoses, even when the final diagnosis is benign.
This is not a theoretical benefit. Structured differential diagnosis documentation directly addresses the most common allegation in EM malpractice claims: that the physician failed to consider an alternative diagnosis.
Quick Comparison — Top AI Scribes for Emergency Medicine
| Rank | Tool | Price | EM-Specific | CDS | EHR | Best For |
|---|---|---|---|---|---|---|
| 1 | DeepCura | $129/mo | CDS + Evidence + Procedures | Differentials | 9 (bidirectional) | Best Overall |
| 2 | Freed AI | $39-$104/mo | General-purpose | None | Scraping-based | Simplest Ambient |
| 3 | Abridge AI | Enterprise | Published EM study | None | Epic-native | Health System EDs |
| 4 | Nuance DAX Copilot | $369+/mo | General + Epic | None | 40+ (deepest Epic) | Enterprise EDs |
| 5 | DeepScribe | ~$99-$149/mo | Customizable templates | None | Limited | Budget Ambient |
| 6 | Ambience Healthcare | Enterprise | Health system deployments | None | Enterprise | Large Health Systems |
For a broader comparison across all specialties, see our Best AI Medical Scribes in 2026 ranking.
What to Look for in an Emergency Medicine AI Scribe
Not all AI scribes can handle the pace, complexity, and medicolegal stakes of emergency medicine documentation. Before choosing a tool, evaluate it against these eight criteria:
1. Speed and Throughput Matching. ED visits last 15-45 minutes and physicians see 2-4 patients per hour. Notes must be generated and finalized before the next patient — ideally within 60 seconds of encounter completion. An AI scribe that takes 5 minutes to produce a draft breaks the ED workflow. Speed is not a luxury in emergency medicine; it is a core requirement.
2. Clinical Decision Support. Differential diagnoses are the safety net that protects against missed diagnoses — EM's number one malpractice risk. The AI should flag critical differentials: PE in chest pain with tachycardia, subarachnoid hemorrhage in thunderclap headache, ectopic pregnancy in reproductive-age women with abdominal pain. CDS integrated into the documentation workflow transforms a scribe from a typing tool into a clinical partner.
3. MDM Documentation for E&M Coding. Proper coding for 99281-99285 requires structured documentation of data reviewed (labs, imaging, outside records), number and complexity of diagnoses addressed, and management complexity including risk of morbidity and mortality. The AI must structure MDM elements to support the E&M level billed — not bury them in narrative prose.
4. Procedure Note Generation. Emergency physicians perform procedures constantly: intubation, central line placement, chest tube insertion, laceration repair, procedural sedation, lumbar puncture, fracture reduction, abscess drainage. Each procedure has required documentation elements — informed consent, timeout, patient identification, technique and approach, medications administered, complications or lack thereof, and post-procedure assessment. An AI scribe without procedure note templates forces manual documentation for some of the ED's most time-consuming charting.
5. Multi-System Encounter Handling. Undifferentiated patients present to the ED with overlapping symptoms across multiple organ systems. A patient with chest pain may require cardiac, pulmonary, GI, and musculoskeletal documentation in a single encounter. The AI must document the full workup across systems without losing clinical coherence or generating fragmented notes.
6. Evidence-Based Medicine Integration. The ability to search PubMed, clinical guidelines, and FDA drug labels at the bedside during documentation transforms the AI scribe from a charting tool into a clinical decision partner. Emergency physicians frequently encounter unfamiliar presentations, rare drug interactions, and guideline-sensitive decisions that benefit from real-time evidence access.
7. EHR Integration. Bidirectional write-back to Epic, Cerner, athenahealth, and other ED information systems is essential. Notes must flow into the chart before shift change — not sit in a separate application waiting for manual transfer. Speed of EHR integration matters as much as integration depth in the emergency department.
8. Disposition and Handoff Documentation. Structured discharge instructions, admission handoffs (I-PASS framework), transfer documentation, and boarding patient reassessments require specific formatting. The AI should support handoff communication standards endorsed by the Joint Commission and generate disposition documentation that meets both clinical and regulatory requirements.
Detailed Reviews
1. DeepCura — Best Overall for Emergency Medicine
DeepCura is a full-stack clinical AI platform combining ambient scribing with clinical decision support, evidence search, practice automation, and bidirectional EHR integration — $129/month with unlimited notes.
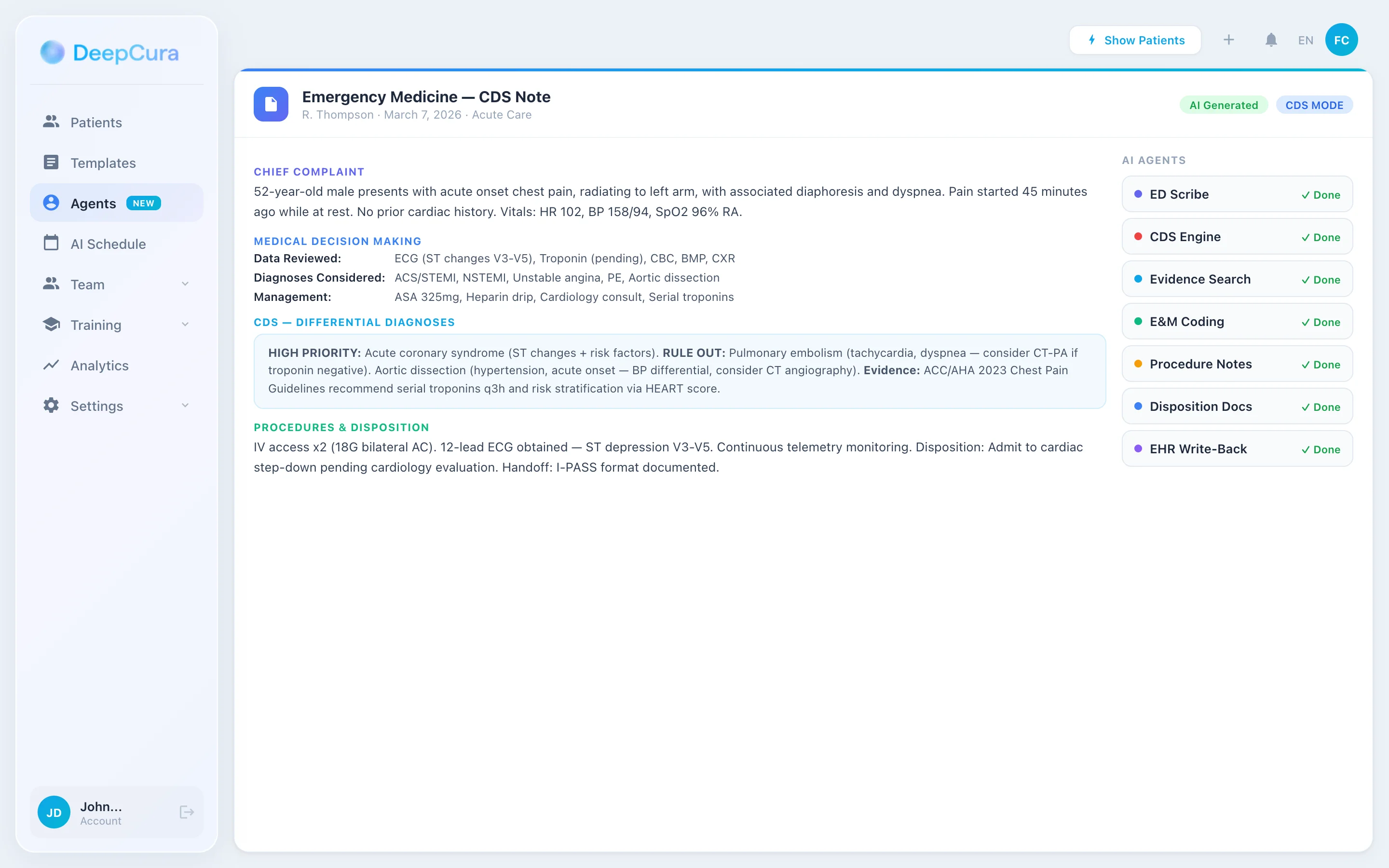
For emergency medicine, DeepCura's key differentiator is CDS Mode: when activated (3 credits), the AI generates differential diagnoses alongside the clinical note, flagging critical "can't miss" diagnoses and suggesting workup validation. No other AI scribe integrates clinical decision support directly into the documentation workflow. For the emergency physician worried about missing a PE in a chest pain patient or an ectopic in an abdominal pain presentation, CDS Mode provides a systematic second check built into every note.
DeepEvidentia — DeepCura's evidence search engine — lets EM physicians query PubMed, Google Scholar, and FDA drug labels mid-encounter. "Should I give TXA for this GI bleed?" returns instant citations with adaptive depth. "What is the Wells score threshold for CTPA in suspected PE?" surfaces guideline-level evidence in seconds. This transforms documentation time into clinical decision-making time.
Strengths:
- CDS Mode with differential diagnoses (GPT-5, 3 credits per note)
- DeepEvidentia evidence search (PubMed/Scholar/FDA at bedside)
- Multiple AI models matched to encounter acuity (1-15 credits)
- Procedure note templates for ED procedures (intubation, central line, chest tube, laceration repair, procedural sedation, lumbar puncture)
- Bidirectional EHR write-back across 9 systems (Epic, Cerner, athenahealth, eClinicalWorks, AdvancedMD, Veradigm, CharmHealth, OptiMantra, browser-based)
- AI receptionist for post-discharge follow-up calls
- Billing automation with E&M coding integrity checks for 99281-99285
- Unlimited notes on all plans
Limitations:
- CDS Mode costs additional credits (3 per note vs. 1 for standard)
- No pre-built trauma-specific templates (available via custom template builder)
Pricing: $129/month per provider — all features included. Free trial available, no credit card required.
Verdict: DeepCura is the strongest choice for emergency physicians who want clinical decision support integrated into their documentation workflow. The CDS differential diagnosis feature is unique in the market and directly addresses EM's number one malpractice risk: missed diagnoses. At $129/month with unlimited notes, procedure note templates, evidence search, and 9-system EHR integration, it offers the most complete emergency medicine documentation solution available.
DeepCura: AI Scribe with Clinical Decision Support
CDS differentials, evidence search, procedure notes, E&M coding, and bidirectional EHR integration — $129/mo, unlimited notes. Start your free trial.
+1 (415) 549-1829Available 24/7 · Set up in seconds · No credit card required
2. Freed AI — Simplest Ambient Scribe for the ED
Freed AI is the most streamlined ambient scribe on the market — click record, see your encounter, get a note. Minimal setup, clean interface, and a learning curve measured in minutes rather than hours. For emergency physicians who want documentation without complexity, Freed delivers.
For the ED, Freed captures encounters through passive ambient listening and generates SOAP notes quickly. The AI handles general emergency medicine content and produces clean, readable notes. However, Freed does not offer clinical decision support, evidence search, or procedure note templates. EHR integration works through browser-based scraping rather than native API write-back, meaning notes are pushed into the chart via screen overlay rather than written directly to structured EHR fields.
The tiered pricing makes Freed accessible: $39/month for 40 notes on Starter, $79/month for unlimited notes on Core, and $104/month for unlimited notes with EHR push and ICD-10 coding on Premier.
Pricing: $39/month (Starter, 40 notes), $79/month (Core, unlimited), $104/month (Premier, unlimited + EHR push + ICD-10).
Verdict: Best for EM docs who want dead-simple ambient documentation without bells and whistles. Not ideal for those who need CDS, procedure notes, or structured MDM documentation. Read our Freed AI review.
3. Abridge AI — Best for Health System EDs
Abridge has published research on AI documentation in emergency departments, making it one of the few platforms with EM-specific validation data. That published evidence is a meaningful differentiator for health system chief medical officers evaluating AI scribe deployments for their emergency departments.
Abridge captures ED encounters through ambient listening with linked evidence — AI-generated citations from the clinical conversation mapped to note content. This transparency feature lets clinicians verify that each note element traces back to something actually said during the encounter, which is particularly valuable in the high-liability emergency medicine environment.
Strong Epic integration makes Abridge a natural fit for health system EDs already embedded in the Epic ecosystem. The platform is designed for enterprise deployment with institutional-grade security and compliance controls.
Pricing: Enterprise custom — not publicly disclosed. Requires institutional procurement.
Verdict: Best for health system emergency departments on Epic who want published EM validation data and enterprise-grade integration. Pricing and procurement requirements exclude independent EM groups and smaller practices. Read our Abridge AI review.
4. Nuance DAX Copilot — Enterprise Emergency Departments
Nuance DAX Copilot (Microsoft) is the enterprise ambient documentation standard with the deepest EHR integration in the market — compatible with 40+ systems including Epic, Cerner, and athenahealth. For hospital-based emergency departments, DAX offers seamless integration within existing EHR workflows and institutional-grade security backed by Microsoft.
DAX handles ED encounters through ambient listening and generates notes within your EHR. Documentation quality for emergency medicine is solid within Epic-native templates, and the Microsoft backing ensures long-term enterprise support and continued development investment. For hospital EDs that have already standardized on Microsoft/Nuance products, DAX integrates into the existing technology stack without friction.
The tradeoff is cost: DAX starts at $369/month per provider plus a $700 one-time implementation fee. There is no CDS or evidence search capability — DAX is a documentation tool, not a clinical decision support platform.
Pricing: $369/month per provider (Solo/Group) + $700 one-time implementation. Enterprise volume discounts available.
Verdict: The default for hospital EDs embedded in Epic with enterprise procurement budgets. The $369+ price point makes it impractical for independent EM groups or democratic groups managing their own overhead. See our Nuance DAX comparison.
5. DeepScribe — Ambient AI for EM
DeepScribe offers ambient AI documentation with customizable templates that can be adapted for emergency medicine workflows. The platform captures encounters passively and generates structured notes based on the clinical conversation.
DeepScribe's template flexibility allows EM groups to build custom note structures that match their departmental documentation standards. The AI handles ambient capture reasonably well, and the mid-range price point makes it accessible for smaller EM groups and independent practices.
However, DeepScribe lacks clinical decision support, evidence search, and purpose-built procedure note templates. EHR integration is more limited than DeepCura's 9-system bidirectional coverage or Nuance DAX's 40+ system compatibility.
Pricing: ~$99-$149/month range.
Verdict: Solid mid-range ambient option with template flexibility for EM groups that want to customize their documentation workflow. Limited EM-specific features compared to DeepCura's CDS approach. Read our DeepScribe review.
6. Ambience Healthcare — Health System Focus
Ambience Healthcare targets large health system deployments with AutoScribe ambient documentation and Chart Awareness context engine. The platform is designed for enterprise-scale implementations with custom integrations tailored to institutional workflows.
For emergency departments within large health systems, Ambience offers institutional-grade ambient documentation with dedicated implementation support. The Chart Awareness engine provides clinical context from the patient's existing medical record during documentation, which can improve note quality for patients with complex medical histories presenting to the ED.
Pricing: Enterprise custom — requires institutional procurement.
Verdict: For large health systems with dedicated IT teams, enterprise procurement budgets, and the infrastructure to support custom AI implementations. Not accessible to independent EM practices, democratic groups, or community hospital EDs without enterprise-level resources. Read our Ambience Healthcare review.
Head-to-Head — Emergency Medicine Documentation Features
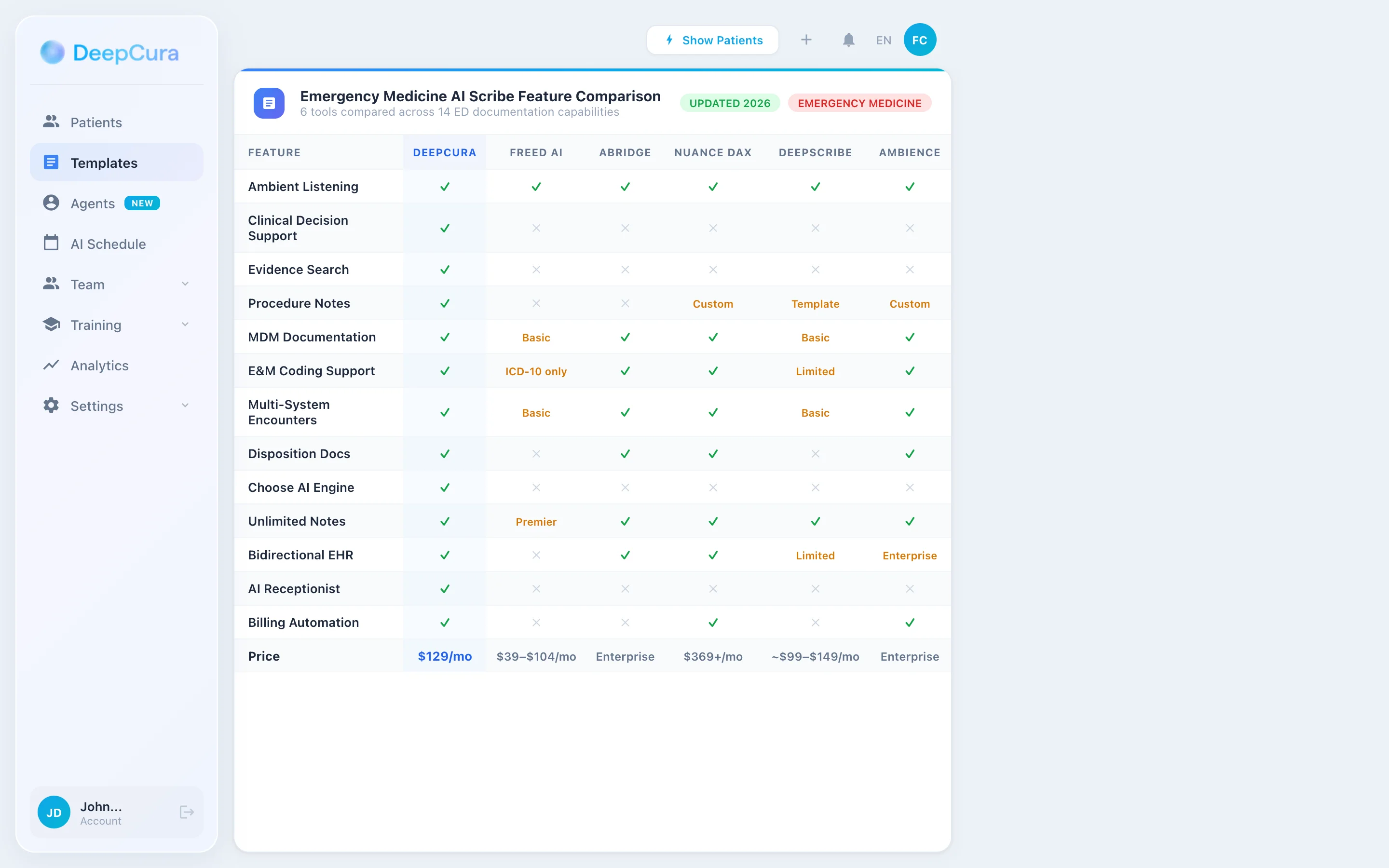
| Feature | DeepCura | Freed AI | Abridge | Nuance DAX | DeepScribe | Ambience |
|---|---|---|---|---|---|---|
| Ambient Listening | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Clinical Decision Support | ✓ (differentials) | ✗ | ✗ | ✗ | ✗ | ✗ |
| Evidence Search | ✓ (DeepEvidentia) | ✗ | ✗ | ✗ | ✗ | ✗ |
| Procedure Notes | ✓ | ✗ | ✗ | Custom | Template | Custom |
| MDM Documentation | ✓ (structured) | Basic | ✓ | ✓ | Basic | ✓ |
| E&M Coding Support | ✓ (99281-99285) | ICD-10 only | ✓ | ✓ | Limited | ✓ |
| Multi-System Encounters | ✓ | Basic | ✓ | ✓ | Basic | ✓ |
| Disposition Documentation | ✓ | ✗ | ✓ | ✓ | ✗ | ✓ |
| Choose AI Engine | ✓ | ✗ | ✗ | ✗ | ✗ | ✗ |
| Unlimited Notes | ✓ | Premier | ✓ | ✓ | ✓ | ✓ |
| Bidirectional EHR | ✓ (9 systems) | ✗ | ✓ (Epic) | ✓ (40+) | Limited | Enterprise |
| AI Receptionist | ✓ | ✗ | ✗ | ✗ | ✗ | ✗ |
| Billing Automation | ✓ | ✗ | ✗ | ✓ | ✗ | ✓ |
| Price | $129/mo | $39-$104/mo | Enterprise | $369+/mo | ~$99-$149/mo | Enterprise |
EM Documentation Workflow with DeepCura
DeepCura's tiered credit system lets emergency physicians match AI resources to encounter complexity — ensuring fast turnaround for simple cases without sacrificing depth for complex presentations.
Fast Track (1 Credit) — URI, Laceration, UTI
For straightforward fast track encounters — upper respiratory infections, simple lacerations, urinary tract infections, ankle sprains — the 1-credit model generates notes in under 30 seconds. Speed-optimized for high-volume fast track where the goal is accurate documentation at maximum throughput. No CDS overhead for encounters where the diagnosis is clinically obvious and the differential is narrow.
Acute Care (3 Credits CDS) — Chest Pain, Stroke, Sepsis
For undifferentiated acute presentations — chest pain, altered mental status, suspected stroke, sepsis — CDS Mode activates differential diagnosis generation alongside the clinical note. The AI flags critical "can't miss" diagnoses, validates that the documented workup addresses the key differentials, and structures MDM to support the appropriate E&M level. This is where the emergency medicine AI scribe earns its value: turning documentation into a clinical safety check.
Critical Care (15 Credits) — Trauma, Complex Multi-System
For complex multi-system encounters — major trauma resuscitations, multi-organ failure, diagnostic puzzles with extensive workups — the maximum-depth model provides comprehensive documentation with full procedure notes, detailed MDM, and thorough differential diagnosis analysis. The higher credit cost reflects the greater reasoning depth required for encounters where documentation complexity matches clinical complexity.
Match AI to Encounter Acuity
1 credit for fast track, 3 credits for CDS differentials, 15 credits for critical care — DeepCura scales documentation depth to match clinical complexity. Start your free trial.
+1 (415) 549-1829Available 24/7 · Set up in seconds · No credit card required
Clinical Decision Support and Evidence Search
CDS Mode — Differential Diagnoses as a Safety Net
The number one cause of EM malpractice claims is missed diagnosis. Not procedural complications, not medication errors — missed diagnosis. CDS Mode directly addresses this risk by generating differential diagnoses with every note, creating a systematic documentation trail that the physician considered and evaluated alternative diagnoses.
When CDS Mode is activated, the AI analyzes the clinical encounter and generates a differential diagnosis list alongside the standard clinical note. Critical "can't miss" diagnoses are flagged prominently — PE in the chest pain patient with tachycardia and recent immobilization, subarachnoid hemorrhage in the patient with worst-headache-of-life, ectopic pregnancy in the reproductive-age woman with abdominal pain and vaginal bleeding.
Evidence validation cross-references clinical findings against known presentations, surfacing clinical pearls at decision points. The system documents not just what the physician diagnosed, but what they considered and why they ruled out high-risk alternatives — exactly the documentation that defense attorneys look for in malpractice cases.
No competitor integrates clinical decision support into the scribe workflow. Freed AI, Abridge, Nuance DAX, DeepScribe, and Ambience are all documentation-only tools that capture what was said and structure it into a note. DeepCura is the only platform that adds a clinical reasoning layer on top of the documentation.
DeepEvidentia — Evidence at the Bedside
DeepEvidentia is DeepCura's integrated evidence search engine, providing real-time access to PubMed, Google Scholar, and FDA drug labels directly within the documentation workflow. For emergency physicians who frequently encounter unfamiliar presentations, rare drug interactions, and guideline-sensitive decisions, bedside evidence access transforms documentation time into clinical decision-making time.
Example queries and what they return:
- "Should I give TXA for this GI bleed?" — instant citations with level of evidence from relevant clinical trials
- "What is the Wells score threshold for CTPA in suspected PE?" — guideline-level evidence with source references
- "Ketamine dose for procedural sedation in a 90kg adult" — FDA label dosing with contraindication checks
Adaptive depth lets physicians control the scope of the evidence search: basic fact lookup (1 credit) for quick reference questions, comprehensive literature review (5 credits) for complex clinical decisions. Contraindication detection flags drug-drug and drug-condition interactions relevant to the current encounter.
DeepEvidentia transforms the AI scribe from a documentation tool into a clinical decision partner — the difference between an AI that types what you said and an AI that helps you think through what to do.
Pricing Comparison
| Tool | Monthly | Note Limit | CDS | Best Plan |
|---|---|---|---|---|
| DeepCura | $129/mo | Unlimited | ✓ (3 credits/note) | Single plan, all features |
| Freed AI | $39-$104/mo | 40-unlimited | ✗ | Core ($79) or Premier ($104) |
| Abridge AI | Enterprise | Unlimited | ✗ | Custom health system pricing |
| Nuance DAX | $369+/mo | Unlimited | ✗ | Solo ($369) or Enterprise |
| DeepScribe | ~$99-$149/mo | Unlimited | ✗ | Standard plan |
| Ambience | Enterprise | Unlimited | ✗ | Custom health system pricing |
See DeepCura in Action
Watch how DeepCura handles the full clinical workflow — from AI receptionist calls and patient intake through ambient scribing with CDS, automated billing, and native EHR write-back.

Frequently Asked Questions
What is the best AI scribe for emergency medicine?
DeepCura is the best overall AI scribe for emergency medicine in 2026. It is the only platform that integrates clinical decision support (differential diagnoses) directly into the documentation workflow — addressing EM's number one malpractice risk of missed diagnoses. At $129/month with unlimited notes, CDS mode, evidence search via DeepEvidentia, procedure note templates, and bidirectional EHR integration across 9 systems, it offers the most complete emergency medicine documentation solution available.
Can AI scribes handle ED procedure notes?
Yes, but support varies significantly. DeepCura generates structured procedure notes for common ED procedures including intubation, central line placement, chest tube insertion, laceration repair, procedural sedation, and lumbar puncture — with required documentation elements (informed consent, timeout, technique, complications, post-procedure assessment). Nuance DAX supports procedure notes through custom Epic templates. Most other AI scribes (Freed AI, DeepScribe) do not have built-in procedure note capabilities, requiring physicians to document procedures manually.
Do AI scribes work with Epic in the emergency department?
Yes. Nuance DAX Copilot has the deepest Epic integration with full ambient capture and note generation within the Epic workflow — compatible with 40+ EHR systems total. DeepCura offers bidirectional Epic integration via FHIR R4 for notes, diagnoses, allergies, medications, and billing codes. Abridge also has strong Epic integration designed for health system deployments. Freed AI uses browser-based scraping rather than native Epic API integration, which means notes are pushed via screen overlay rather than written to structured EHR fields.
How do AI scribes handle high-volume ED documentation?
The best AI scribes for the ED generate notes in under 60 seconds, matching the rapid pace of emergency medicine where physicians see 2-4 patients per hour. DeepCura's tiered credit system lets physicians match AI resources to encounter complexity — 1 credit for fast track visits (note in under 30 seconds), 3 credits for acute care with CDS differential diagnoses, and 15 credits for complex critical care encounters requiring maximum documentation depth. This ensures fast turnaround for simple cases without sacrificing clinical depth for complex presentations.
Is ambient AI listening accurate in noisy EDs?
Modern AI scribes use noise cancellation and speaker diarization to separate clinician-patient conversation from background ED noise. Accuracy depends on microphone placement and proximity to the conversation. Most platforms recommend a lapel microphone or phone placement within 3-4 feet of the speakers. Background noise from cardiac monitors, overhead pages, adjacent bays, and equipment alarms can impact transcription accuracy — verify performance during your trial period in your actual ED environment, not in a quiet office.
Do AI scribes support clinical decision support for EM?
Currently, DeepCura is the only AI scribe that integrates clinical decision support directly into the documentation workflow. CDS Mode generates differential diagnoses alongside the clinical note, flagging critical "can't miss" diagnoses for emergency physicians. No other ambient AI scribe — including Freed AI, Abridge, Nuance DAX, DeepScribe, or Ambience Healthcare — offers integrated CDS with differential diagnosis generation. This is a meaningful gap in the market given that missed diagnosis is the leading cause of EM malpractice claims.
How much does an AI scribe for emergency medicine cost?
Pricing ranges from $39/month to enterprise custom. Freed AI starts at $39/month (Core at $79, Premier at $104 with EHR push and ICD-10). DeepScribe costs approximately $99-$149/month. DeepCura is $129/month with unlimited notes, CDS, evidence search, procedure notes, and 9-system EHR integration. Nuance DAX starts at $369/month plus a $700 implementation fee. Abridge and Ambience require enterprise procurement with custom pricing. For most independent EM groups, the $99-$129/month range offers the best feature-to-cost ratio.
Can AI scribes document boarding patient reassessments?
Boarding patient reassessments require interval documentation of clinical status changes, repeated physical exams, and ongoing management decisions — sometimes spanning hours or days while admitted patients wait for inpatient beds. DeepCura and Nuance DAX support sequential encounter documentation where the AI maintains clinical context across reassessment intervals, allowing physicians to document interval changes without re-establishing the full clinical picture each time. Most other AI scribes treat each recording as an independent encounter, requiring the physician to re-establish context manually for each reassessment.
Final Verdict
For emergency physicians and EM groups, the choice comes down to three profiles:
Best overall: DeepCura at $129/month — CDS differentials, evidence search, procedure notes, 9-system EHR integration, unlimited notes. The only platform addressing EM's number one malpractice risk (missed diagnosis) directly through integrated clinical decision support. For independent EM groups, democratic groups, and community hospital EDs, this is the strongest feature-to-cost ratio in the market.
Best simplicity: Freed AI at $79/month — dead-simple ambient documentation for EM docs who want clean notes without practice automation, CDS, or procedure note templates. The fastest learning curve of any AI scribe, with a clean interface that stays out of your way.
Best enterprise: Nuance DAX Copilot at $369+/month — the deepest Epic integration for hospital EDs with enterprise procurement budgets and institutional standardization requirements. The default for health system EDs where Epic compatibility and Microsoft enterprise support are non-negotiable.
For a broader comparison across all specialties, see our Best AI Medical Scribes in 2026 ranking. For lower-acuity walk-in workflows including laceration repair, splinting, work-comp DWC forms, DOT exams, and sports physicals, see our best AI scribe for urgent care guide. For ER nursing triage, ESI acuity assignment, and SBAR handoff documentation, see our best AI scribe for nurses ranking. For PA-led emergency department coverage and allied health workflows, see our best AI scribe for medical professionals guide. For clinical AI chat tools that support emergency medicine decision-making, see Best ChatGPT for Doctors. For practices that need phone automation alongside documentation, see our Best AI Medical Receptionist guide. For psychiatry-specific documentation, see our best AI scribe for psychiatry guide. For a comparison of traditional dictation vs. ambient AI tools with pricing and free tiers, see our 15 best medical dictation software guide. For AI vs. traditional transcription services, see our best medical transcription software comparison. If you are choosing an EHR for a small practice, see our best EMR for small practices ranking. And for free copy-paste clinical note templates, see our SOAP note template guide.
References
[1] American College of Emergency Physicians, "ACEP Report on Emergency Medicine Documentation Burden," ACEP.org. acep.org
[2] American Medical Association, "Physician Burnout and Well-Being: The AMA Physician Health and Resiliency Resources," AMA. ama-assn.org/practice-management/physician-health
[3] Annals of Emergency Medicine, "Time-Motion Studies of Emergency Physician Workflow and Documentation," Annals of Emergency Medicine. annemergmed.com
[4] Centers for Medicare & Medicaid Services, "Evaluation and Management (E/M) Visit Coding — CPT Codes 99281-99285," CMS.gov. cms.gov/medicare/payment/prospective-payment-systems
[5] Agency for Healthcare Research and Quality, "Diagnostic Errors in the Emergency Department," AHRQ Patient Safety Network. psnet.ahrq.gov
[6] The Joint Commission, "Sentinel Event Alert: Inadequate Hand-off Communication — I-PASS Framework," Joint Commission. jointcommission.org
[7] U.S. Department of Health and Human Services, "HIPAA for Professionals," HHS.gov. hhs.gov/hipaa/for-professionals
[8] DeepCura, "AI Medical Scribe Platform — Ambient Scribing, CDS, AI Receptionist, EHR Integration," DeepCura.com. deepcura.com
[9] CRICO/Harvard, "Comparative Benchmarking System — Emergency Medicine Malpractice Claims Analysis," CRICO. rmf.harvard.edu
[10] Medscape, "Physician Compensation and Burnout Report 2026 — Emergency Medicine," Medscape. medscape.com